Instruction
1
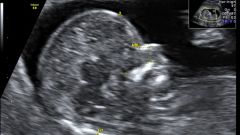
Second ultrasound - the most anticipated by parents, they will be able to see a child look like a little person. A limb is formed, the front part of the skull too. If the monitor is configured well, few moms can hide the tears of emotion: the child sucks fingers, tumbles, actively yawns and smiles. Today doing a 3D ultrasound, in this case, the image rendering will be more accurate, and the doctor is able to examine the child in detail.
2
If the doctor is suspected pathology of pregnancy or pathology of the fetus, the woman is administered an ultrasound on 20-21 week the experts had the opportunity to appoint additional studies ─ for example, cordocentesis, and the mother accepted the decision on continuation of the pregnancy. In this period already well the types of defects, incompatible with life, leading to severe consequences.
3
The doctor will look at the condition of the child. He will conduct measurements of the limbs, internal organs, will calculate the estimated weight of the child will count the number of fingers on the hands and feet. All data will be recorded in the minutes. Sometimes the ultrasound showed one limb is shorter than the other by several mm ─ it's not a sign of disturbance, the child is in motion, because the slight distortion of the result.
4
Is evaluated and the condition of the placenta: the place of its attachment, the size, the availability of additional shares features of structure, anomalies, circulation. Together with the placenta assessment of the umbilical cord. Examines the number of vessels in the umbilical cord and features of the circulation. If the umbilical cord is short, it may be a problem: the baby passing through the birth canal will pull the placenta, which is not yet ready to secede. These women typically operate. Too long umbilical cord, the child may become tangled, the part of the umbilical cord might fall, there can be nodes. Especially dangerous is your node and double tight entanglement neck ─ the blood supply to the baby and possible intrauterine death. Such women need weekly monitoring to be able to resort to emergency delivery. According to who, since 24 weeks, the viability of the fetus is very high, and with each subsequent week the percentage of survival increases.
5
At this period a visible amniotic fluid. The doctor is able to accurately identify their pathology: oligohydramnios, polyhydramnios. Pronounced oligohydramnios ─ a dangerous symptom, it can indicate leakage of water, intrauterine infection and other dysfunctional States. Polyhydramnios in this respect are less dangerous, but increases the likelihood of entanglement of the umbilical cord and loss of body parts or placenta in childbirth. The doctor will look at the state of the cervix, or rather, her internal OS. The throat should be closed. If the inner throat is open, there is a risk of premature birth.
6
The approximate weight of the fetus at this period of 250-300 g, long ─ 16-18 see Should abandon the self-interpretation of ultrasound data. As an obstetrician evaluates them in conjunction, courteous average data for the population, as well as boundary values. The fruit can grow in leaps and bounds and most objective information about the normal blood circulation and normal development of internal organs. During this period begins to have the value of the individual characteristics of parents ─ the parents and the child will be large, and lean and low growth is unlikely to be born 4-pound athlete.
7
The second ultrasound lasts about 20-30 minutes, if multiple pregnancy, the study lasts longer. Immediately after the ultrasound, she should be referred to the office, where they will do an ECG of the fetus. Almost all complications, with the exception of defects incompatible with life and complex anomalies of the placenta, it is possible to compensate correctly chosen treatment because you should not neglect ultrasound diagnostics.
Note
Must have a puncture the previous ultrasound, in the absence of ─ the direction of a physician, passport, insurance, spare shoes or Shoe covers, a diaper and wipes.
Useful advice
If you want to know the sex of the child, inform the doctor-diagnostician. Not all parents want to know in advance the sex of a baby.